ResMed AirSense 10: A Comprehensive Review and Guide
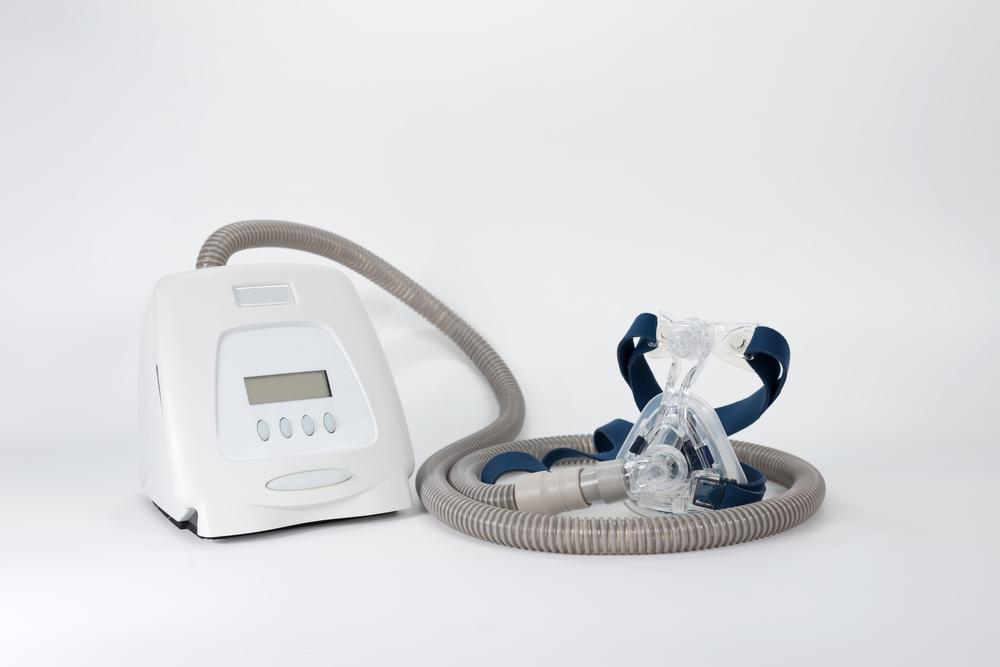
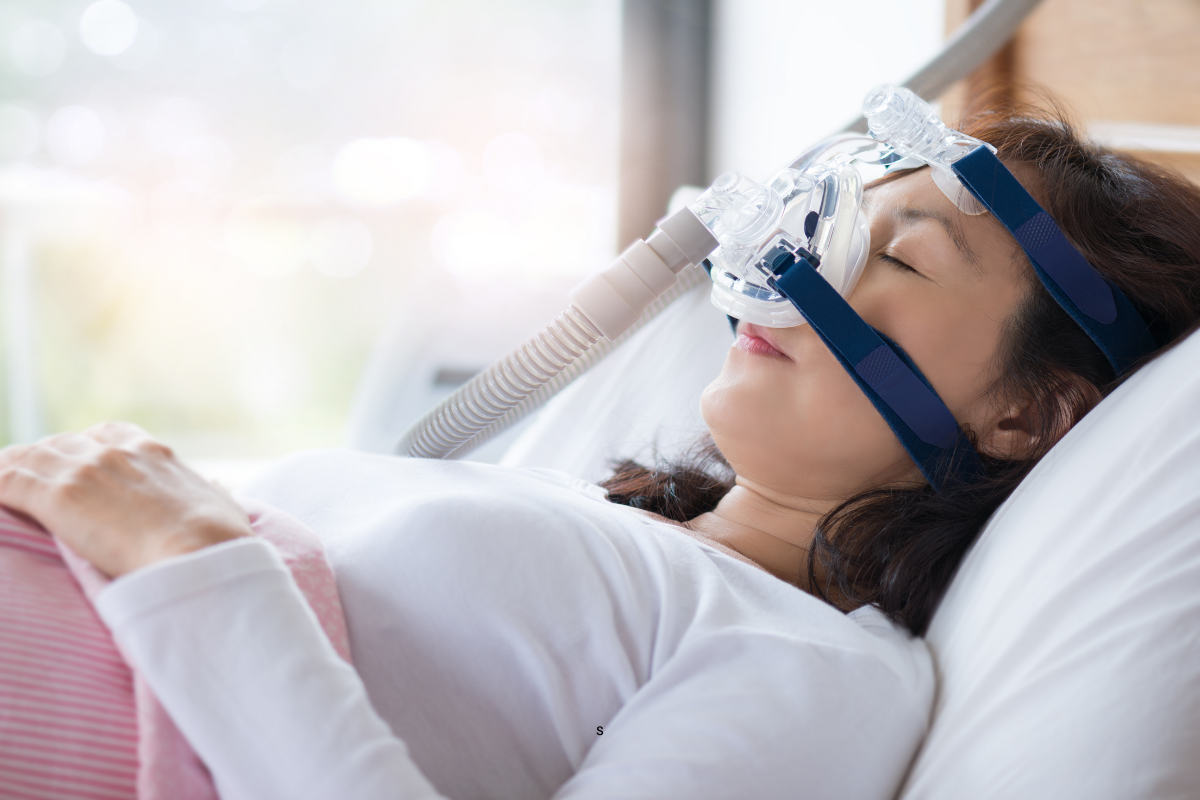
In this comprehensive review and guide, we will take an in-depth look at the ResMed AirSense 10, a popular and highly regarded CPAP device. Designed to provide effective relief for sleep apnea and other breathing disorders, the AirSense 10 offers …
ResMed AirSense 10: A Comprehensive Review and Guide Read more »